CPR: A Step-by-Step Guide (What to do - exactly - when every second counts)
Introduction
Cardiopulmonary resuscitation (CPR) is the emergency procedure performed when a person collapses and is unresponsive or not breathing normally. CPR keeps oxygenated blood moving to the brain and vital organs until trained help or a defibrillator (AED) is available. Early, high-quality chest compressions greatly increase the person’s chance of survival — which is why knowing what to do, and doing it confidently, matters. This page gives you clear, no-skip steps for recognising cardiac arrest, calling for help, giving chest compressions and rescue breaths (when trained), using an AED, and caring for children and infants. (Key clinical guidance summarized from major resuscitation authorities.)
1. Recognise the emergency: How to tell if someone needs CPR
First, quickly check whether the person is responsive and breathing. Approach safely, tap their shoulders and shout, “Are you okay?” Look for normal breathing — not gasping or occasional agonal breaths. If they do not respond and are not breathing normally, treat this as cardiac arrest and start CPR immediately. Do not waste time checking a pulse unless you are trained and confident to do so — lay rescuers should focus on responsiveness and breathing. Recognising arrest early shortens the time without blood flow and improves outcomes. If you are unsure, treat the person as if they need CPR and start compressions.
2. Call for help: who to contact and what to say
If you are alone and find an unresponsive person who isn’t breathing normally, call your local emergency number immediately (for India: 112 or your regional emergency number). If help is nearby, shout for a bystander to call emergency services and to bring an AED if one is accessible. If someone else is calling, tell them exactly where you are, what happened, the victim’s condition (unconscious and not breathing normally), and ask them to bring an AED and meet you. If you are alone and must call, put the phone on speaker and follow dispatcher instructions while you begin CPR — emergency dispatchers can coach you through chest compressions step by step. Early activation of emergency services plus CPR is the most effective combination to save a life.
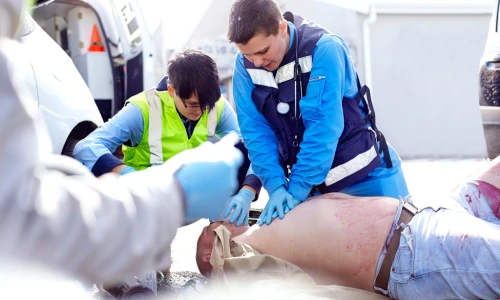
3. Start hands-only CPR (for untrained rescuers or if you’re unwilling/unable to give breaths)
If you are not trained in rescue breaths, or you prefer not to give them, begin hands-only CPR immediately. Follow these exact steps in order — do not skip:
Place the person flat on their back on a firm surface.
Kneel at their side and locate the centre of the chest (the lower half of the breastbone/sternum).
Put the heel of one hand on the centre of the chest and place your other hand on top, interlacing fingers. Keep fingers off the ribs and off the chest.
Position your shoulders directly above your hands, keep your elbows straight, and use your upper body (not just your arms) to compress.
Press hard and fast — compress the chest to a depth of about 5–6 cm (2–2.4 inches) for adults, at a rate of 100–120 compressions per minute. Allow the chest to fully recoil (rise) between compressions so the heart can refill.
Do continuous compressions until help arrives or an AED is ready to use — minimize interruptions and do not stop compressions except to use an AED or if the scene becomes unsafe.
If emergency services arrive, follow their instructions; if another trained rescuer takes over, swap roles every 2 minutes if possible to avoid rescuer fatigue.
Hands-only CPR is effective at maintaining blood flow and is recommended for untrained bystanders — starting immediately is critical.


4. Full CPR (compressions + rescue breaths) - step-by-step for trained rescuers
If you are trained and comfortable performing rescue breaths, follow the C-A-B sequence (Compressions → Airway → Breathing). Execute these steps precisely:
Ensure the person is on their back on a firm surface. Kneel beside them.
Start with 30 chest compressions as described above (rate 100–120/min, depth 5–6 cm for adults). Count aloud (1…2…3…) to maintain pace.
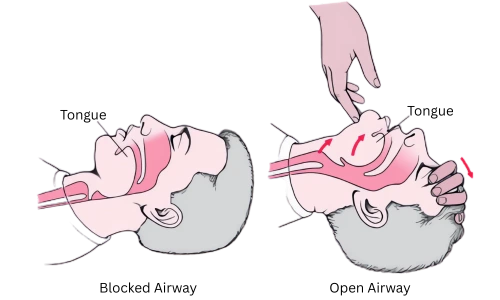
After 30 compressions, open the airway using the head-tilt, chin-lift maneuver: place one hand on the forehead and two fingers on the chin, tilt the head back gently (unless you suspect neck injury – in that case use a jaw – thrust if trained).
Pinch the nose closed, take a normal breath, make a complete seal over the person’s mouth with yours, and give 2 rescue breaths – each breath over 1 second, watching for the chest to rise. If the chest does not rise, reposition the head and try again.
Resume 30 compressions immediately after the two breaths. Continue cycles of 30 compressions : 2 breaths. Minimize pauses – each pause should be under 10 seconds when possible.
If an advanced airway is in place (only in professional settings), give continuous compressions and provide breaths every 6–8 seconds (approx. 8–10 breaths per minute) without pausing compressions.
Continue until the victim shows signs of life, an AED/defibrillator is ready and used, professional help arrives and takes over, or you are physically unable to continue.
Rescue breaths are critical in cases where the arrest was caused by a breathing problem (drowning, overdose, pediatric cases) – so when trained, include them.
5. How to use an AED (automated external defibrillator) — exact steps
An AED analyses the heart rhythm and delivers a shock if needed; early defibrillation significantly increases survival after sudden cardiac arrest. Use an AED as soon as one is available – here’s precisely how:
- Power the AED on (open the lid or press the ON button). Follow the device voice prompts.
- Expose the person’s bare chest – remove clothing and wipe away sweat or moisture. If chest hair prevents pad adhesion, quickly shave an area if a razor is available (many AED kits include one).
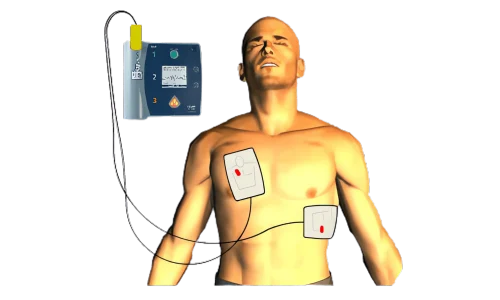
- Apply the adhesive pads as shown on the pads (one pad on the upper right chest below the collarbone; the other pad on the lower left lateral chest). Make sure pads do not touch each other.
- Plug in the connector if required and allow the AED to analyse the rhythm. Stand clear – do not touch the person during analysis.
- If the AED advises a shock, make sure no one is touching the person, shout “CLEAR,” and press the shock button when prompted. After the shock (or if no shock is advised), resume CPR immediately starting with compressions – do not wait.
- Continue following AED prompts and performing CPR until EMS arrives or the person shows clear signs of life.
AEDs are designed for lay rescuers and give step-by-step voice instructions; their early use combined with CPR saves lives.
6. CPR for children and infants - what changes (don’t skip these differences)
Children and infants have different chest sizes and common causes of arrest (often breathing-related), so technique and depth change. For a child (1 year to puberty): use one or two hands (depending on the rescuer’s ability) to compress the lower half of the breastbone about one-third of the chest depth (roughly 5 cm), at 100–120 compressions per minute. If you are alone and the child is not breathing, perform 2 minutes of CPR (about 5 cycles of 30:2) before leaving to call emergency services if no phone is available. For an infant (under 1 year): use two fingers at the center of the chest (just below the nipple line) and compress to about one-third of chest depth (~4 cm) at the same rate; if two rescuers are present, the two-thumb encircling technique is preferred. For infants and children, rescue breaths are especially important – if you are trained, include the 2 breaths after each set of compressions. These differences are important because children’s arrests are often due to respiratory problems rather than primary cardiac causes.

7. Special situations: choking, drowning, pregnancy, trauma, and safety considerations
CPR must be adapted for some special situations. For severe choking (the person cannot breathe, cough or speak), perform a sequence of abdominal thrusts (Heimlich maneuver) for conscious adults and children; if they become unconscious, lower them to the ground, call for help, start CPR, and before breaths check the mouth for dislodged objects and remove with a finger sweep only if you can easily see the object. For drowning, start rescue breaths first if you are trained (oxygenation is critical), then compressions; for pregnant patients, place hands slightly higher on the sternum and if available, manually displace the uterus to the left or tilt the backboard 15-30 degrees to relieve aortocaval compression once advanced help arrives. For trauma (suspected spinal injury), stabilise the neck and only open the airway using jaw-thrust if trained. Always ensure scene safety – do not place yourself at undue risk. In all these situations, begin CPR as soon as the person is confirmed unresponsive and not breathing normally, and get professional help quickly.
8. When to stop CPR and what happens immediately after ROSC (return of spontaneous circulation)
Continue CPR until one of the following happens: a trained rescuer or emergency services take over, you are physically unable to continue, the person shows clear signs of life (breathing normally, moving), or a valid do-not-resuscitate order is presented. After the person regains a pulse (ROSC), place them in the recovery position if breathing and there is no suspected spinal injury, support airway and breathing, monitor for deterioration, and prepare for transport to hospital – post-resuscitation care may include oxygenation, monitoring, and advanced cardiac care. Even if the person appears to recover fully, urgent hospital assessment is essential because underlying causes must be identified and treated.
9. Why step-by-step CPR matters: the science behind every action
Every element of CPR – recognising arrest quickly, activating emergency services, high-quality compressions at the correct depth and rate, minimal interruptions, early defibrillation – is backed by evidence showing improved survival when performed correctly and promptly. Chest compressions maintain circulation; correct depth and full recoil maximise blood flow. The 30:2 compression-to-ventilation cycle balances circulation with oxygenation when rescue breaths are provided. AEDs restore a shockable rhythm in many sudden cardiac arrests. Practicing the steps and knowing how to use an AED reduces hesitation and error during a real emergency. In short: following the sequence exactly – as described on this page – gives the victim the best chance of survival.
10. Training, practice, and preparedness — how to keep skills ready
CPR performance improves with hands-on practice. Attend a certified course that includes manikin practice, AED training, and scenario drills. Refresh skills every 1–2 years as recommended by training organizations. Encourage offices, schools, and community groups to have AEDs installed and staff trained. Practice the mental flow: recognise – call – compress – get AED – continue. Keep a visible plan at home and at work (where is the AED, who calls emergency services, who takes over compressions). The more people know these steps, the sooner someone can act decisively – and sooner action saves lives. Shan Multi Hospital offers regular community CPR and first-aid training to help families and staff stay ready.
